For many people exploring lectins and their impact on health, the conversation often starts in the gut. Symptoms like bloating, discomfort, irregular digestion, brain fog, joint stiffness, or immune flares tend to appear after meals, and the immediate assumption is that something is irritating the intestinal lining itself. While that idea is not entirely wrong, it skips over one of the most important protective systems in the body: the mucus layers that line the digestive tract.
The gut is not a bare tube where food particles scrape directly against sensitive tissue. Instead, it is coated with a complex, living barrier made primarily of mucus. This barrier acts as a buffer between what we eat and the cells responsible for absorption, immune signaling, and repair. Understanding how lectins interact with this mucus layer helps explain why some foods cause problems in some people, why symptoms can be delayed or inconsistent, and why preparation and lifestyle factors matter just as much as food choices themselves.
This is not about labeling lectins as universally harmful. It is about understanding context, exposure, and the biological systems that evolved to manage them.
The Mucus Layer Is More Than Just Slime
Mucus tends to get a bad reputation. Most people think of it as something the body produces when it is sick or inflamed. In reality, mucus is a critical, healthy structure that exists throughout the body, especially in the digestive tract.
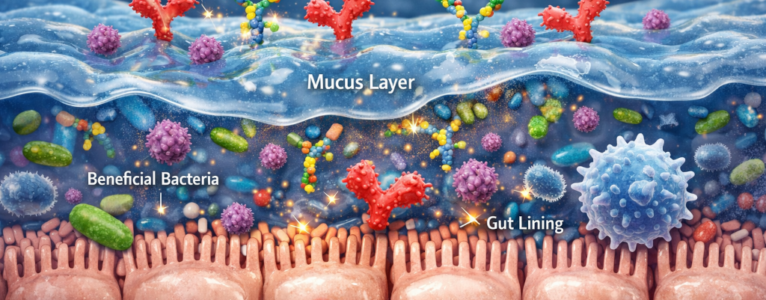
In the gut, mucus is made primarily of large proteins called mucins. These proteins form a gel-like matrix that coats the intestinal lining. This matrix serves several vital functions at once. It physically separates food particles and microbes from the intestinal cells. It houses beneficial bacteria that support digestion and immune balance. It also regulates how substances interact with the gut wall, slowing down or blocking access when needed.
Rather than being a passive coating, the mucus layer is dynamic. It is constantly produced, renewed, and adjusted based on diet, stress, sleep, inflammation, and microbial activity. When functioning well, it acts like a selective filter rather than a wall. Nutrients pass through. Harmful or irritating compounds are slowed, diluted, or redirected.
This is where lectins enter the story.
Why Lectins Are Drawn to Mucus
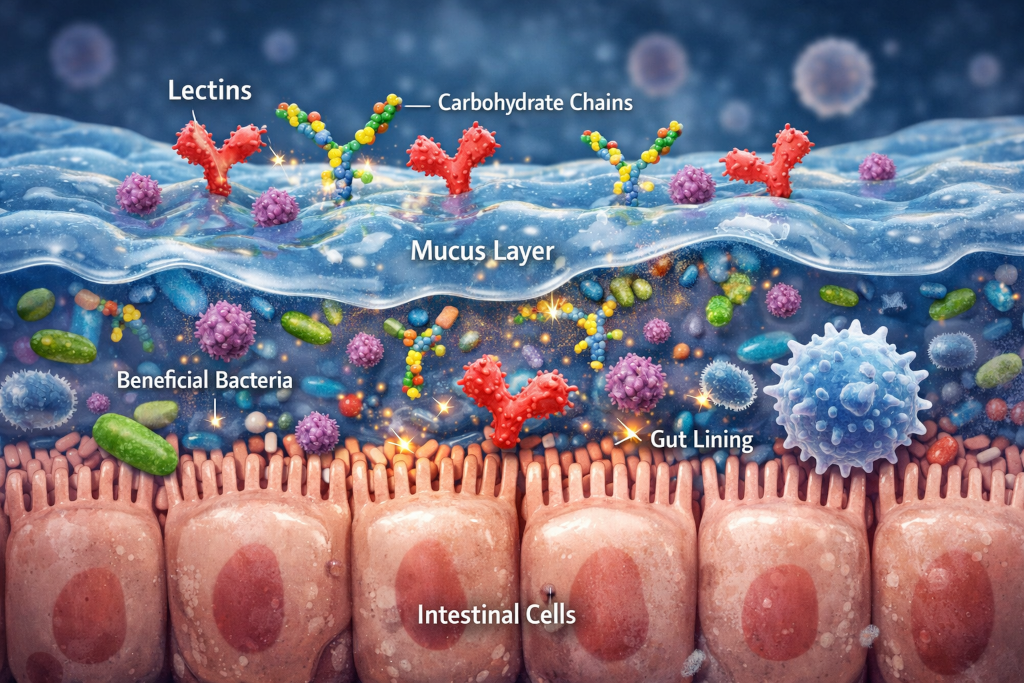
Lectins are carbohydrate-binding proteins. That detail matters more than almost anything else about them.
The mucus layer is rich in complex carbohydrates. Mucins are heavily glycosylated, meaning they are decorated with sugar chains. These sugar structures are not random. They are part of how mucus traps microbes, communicates with immune cells, and maintains balance in the gut ecosystem.
Because lectins bind to specific carbohydrate patterns, they naturally interact with mucus. In many cases, this interaction is protective. Lectins bind to the mucus instead of reaching the intestinal cells beneath it. The mucus acts like a sponge, absorbing and neutralizing lectins before they can cause irritation.
This is one reason why healthy individuals can eat lectin-containing foods without obvious issues. Their mucus layer is robust enough to handle the exposure.
Problems arise when the balance shifts.
When the Mucus Barrier Becomes Vulnerable
The mucus layer is not indestructible. It can thin, become patchy, or change composition under certain conditions. Chronic stress, poor sleep, low fiber intake, dehydration, inflammation, infections, and repeated exposure to irritants can all affect mucus quality.
When mucus production slows or its structure weakens, lectins have fewer places to bind safely. Instead of being intercepted, they can move closer to the intestinal lining. At that point, lectins may interact directly with epithelial cells or immune receptors.
This interaction does not automatically cause damage. But in sensitive individuals, it can trigger localized inflammation, altered permeability, or immune signaling that feels like a reaction.
Importantly, this process helps explain why lectin sensitivity often feels inconsistent. A food that causes symptoms one day may be tolerated another day. The difference is not always the food itself. It can be the state of the mucus barrier at that moment.
Lectins Do Not Destroy Mucus on Contact
One common misconception is that lectins strip away or dissolve the mucus layer outright. That idea oversimplifies what is happening.
Most dietary lectins do not instantly degrade mucus. Instead, they bind to it. This binding can become problematic if exposure is high, repeated, or paired with other stressors. Over time, excessive binding may alter how mucus is structured or renewed, especially if the body is already struggling to maintain it.
Think of mucus as a self-cleaning surface. It is designed to capture and release substances. If the system is overwhelmed, the renewal cycle can slow down. When that happens, old mucus may linger longer, become less effective, or lose its protective qualities.
This is one reason why food preparation methods matter so much.
Cooking and Preparation Change the Interaction
Cooking does not just reduce lectin content in foods. It also changes how lectins behave when they encounter mucus.
Heat, moisture, fermentation, soaking, and pressure cooking can alter the shape of lectin proteins. When a lectin’s structure changes, its ability to bind to carbohydrates often decreases. That means fewer interactions with mucus and less chance of irritation.
This helps explain why traditional food cultures rarely consumed high-lectin foods raw. Beans were soaked and cooked. Grains were fermented. Tubers were heated thoroughly. These practices were not arbitrary. They reduced the biological activity of lectins long before modern science could explain why.
For individuals with compromised mucus layers, preparation becomes even more important. Reducing lectin activity gives the mucus time and space to recover and function properly.
The Role of Gut Bacteria in the Mucus Story
The mucus layer is not sterile. It is home to specific populations of beneficial bacteria that help maintain its structure and thickness.
Some gut microbes feed on components of mucus, but in a balanced system, this is a controlled process that stimulates renewal. Other microbes help produce short-chain fatty acids that signal mucus production and repair.
Lectins can influence this microbial ecosystem indirectly. By binding to mucus, lectins may change which microbes thrive near the gut lining. In a healthy system, this may have little impact. In a disrupted system, it can contribute to imbalance.
This is another reason why gut symptoms linked to lectins often overlap with broader digestive issues. The mucus layer sits at the intersection of diet, microbes, and immunity.
Immune Signaling Happens in the Mucus Layer
A lesser-known role of mucus is immune communication. Immune cells sample what is happening in the mucus before deciding whether to react.
When lectins bind heavily to mucus, they may increase immune exposure to certain carbohydrate patterns. In sensitive individuals, this can amplify immune signaling even without direct tissue damage.
This process helps explain why some people experience systemic symptoms like fatigue, joint discomfort, or brain fog after eating lectin-rich foods. The reaction is not necessarily localized injury. It is immune activation triggered by altered signaling at the mucosal surface.
Understanding this distinction matters because it shifts the goal from eliminating lectins entirely to supporting the systems that manage them.
Supporting Mucus Is a Long-Term Strategy
Focusing only on avoiding lectins can become restrictive and stressful. A more sustainable approach includes supporting mucus production and renewal.
Adequate hydration is foundational. Mucus is largely water. Poor hydration directly affects its thickness and flow.
Dietary fiber, particularly from tolerated vegetables and resistant starches, supports mucus indirectly through microbial activity. Sleep regulates mucus renewal cycles. Chronic sleep deprivation has been shown to impair mucosal barriers throughout the body.
Stress management also plays a role. Stress hormones influence mucus secretion and immune sensitivity. This connection explains why digestive reactions often worsen during emotionally demanding periods even when diet remains unchanged.
These factors do not eliminate lectins, but they strengthen the buffer between lectins and sensitive tissue.
Why Some People Improve Quickly and Others Do Not
One of the most frustrating aspects of lectin-related issues is variability in response. Some people feel better within weeks of dietary changes. Others see slow or inconsistent improvement.
Mucus turnover takes time. In a healthy gut, the mucus layer is renewed regularly. In a compromised system, rebuilding that layer can take weeks or months. During that time, reactions may still occur even as healing progresses.
This reality is often overlooked in online discussions that promise rapid transformation. Understanding the mucus layer encourages patience and a broader view of healing.
Rethinking Lectins Through the Lens of Mucus
Lectins are not invaders attacking an unprotected gut. They are dietary proteins interacting with a complex biological interface designed to handle them.
When that interface is strong, lectins are often neutralized without issue. When it is weakened, the same lectins can contribute to discomfort and inflammation.
This perspective moves the conversation away from fear and toward function. It explains why lectins are widespread in human diets across cultures and why problems tend to emerge under modern conditions that strain the body’s protective systems.
Supporting mucus health does not require perfection. It requires consistency, awareness, and respect for the body’s built-in defenses.
Bringing It Back to the Bigger Picture
The mucus layer is a quiet hero of digestive health. It works continuously, rarely drawing attention unless something goes wrong. Lectins interact with it not as villains but as challenges the system is meant to manage.
By understanding this interaction, it becomes easier to make informed choices without falling into extremes. Cooking methods matter. Lifestyle matters. Stress, sleep, and hydration matter. Food quality and preparation matter.
Lectins are part of the story, but they are not the whole story.
For anyone navigating digestive issues, immune sensitivity, or inflammation, learning how lectins interact with mucus layers offers clarity without oversimplification. It reminds us that the body is not fragile, but it does require support to function as designed.
And that is where real progress begins.